Fibromyalgia, as well as other conditions with “invisible” symptoms, is still considered more as a psychological disorder than a clinical disease, although it implies chronic musculoskeletal pain, widespread fatigue, sleep disturbances and other symptoms which affect the quality of family, social and working life. The frequent misdiagnosis of symptoms is the main problem of the delayed times of diagnosis from physicians, who sometimes consider Fibromyalgia in a “grey zone” between a disease with a definition and a symptomatology – as it is – and the “broken record syndrome” – as it was named till some decades ago from scientific community, to indicate a “all in the patient’s head” condition.
Narrative Medicine was applied in an outpatient clinic of rheumatology in an Italian hospital, to explore the living with Fibromyalgia and understand the real patients and physicians’ needs. A crossing between 16 diaries of patients – 15 women and 1 man 30-55 years old – and the rheumatologist of reference’s parallel charts, from the first encounter and the following 40 days of care.
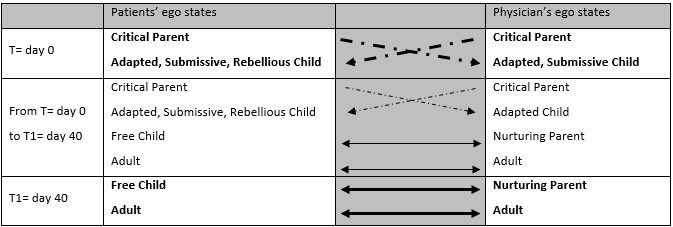
Narratives were analysed using Narrative Medicine classifications and the transactional analysis. From these analysis it was possible “to read” the story of the relationships of care, which usually started with attitudes of reciprocal mistrust: patients didn’t feel believed and recognized in their pain (Adapted and Submissive Child ego state) and in the same time were sceptical toward the therapeutic solutions proposed by the physician (Critical Parent and Rebellious Child ego state); on the other side, the physician doubted about the patients’ suffering (Critical Parent ego state) and felt to be not listened to, sometimes overwhelmed and discouraged (Adapted and Submissive Child ego state). At the end of the first encounter, frustration was the common feeling between patients and doctor.
From patients’ diaries: “My experience with physicians is not the best…My problems of health started when I was 20 years and they had always been underestimated”; “My family doctor explained to me that there are women who suffer from this kind of pain, but they are not worrisome and there is nothing to do”; “I cannot stand too long, or walk too much, because pain becomes intolerable; this changed my life”; “I do not understand why you are telling me I have FIBROMYALGIA! Because I NEVER COMPLAIN, I HATE PEOPLE COMPLYING! I am not at all DEPRESSED”.
From doctor’s parallel charts: “She has a worried and suspicious face. Zero trust physicians, zero trust medicines. She does not open herself to me”; “She is annoyed toward physicians and is very rigid”; “She gives me a bundle full of documents with zillions of exams from the last three years”; “Her pen drive falls over the ground and she bends down to pick it up…didn’t she suffer from backache?!”; “She starts to talk about a series of dubious symptoms”; “Finally I told her that she has fibromyalgia, and she with a hysterical laugh says: “Do not take out the story of fibromyalgia you too! I am not mad! I am not an imaginary sick person!!!”; “I feel pressed, disarmed in front of this flood of words and complains”.
During the following visits, the relationships of care gradually changed and reciprocal trust and understanding was built: patients started to follow the physician’s therapeutic indications, finding improvements, being more open and reducing the wall of mistrust – often originated during years of pilgrimages among centres of care without obtaining answers; the doctor, in the same time, understood through patients’ diaries the real living with Fibromyalgia and gained new elements, which didn’t emerge during the first encounters, to fit the therapeutic plan to their needs. Both became more aware toward the pathway of care and were more comfortable in the relationship (Free Child and Adult ego states).
From patients’ diaries: “I started to feel less tired, my muscles are more released and my daughter also sees me more active. Compared to the time before our encounter, I feel more active. I am happy for how it is going on”; “I feel the pain a little bit less severe. These days are a miracle for me!”.
From doctor’s parallel charts: “She seems more smiling”; “There is a hope to set up a calm and efficient relationship”; “His written story and his tranquillity, perhaps because now he trusts me, helped me to reach the diagnosis. What a nice surprise. Thank you Narrative Medicine!”.
The first result from this pilot experimentation is organizational and economic: 88% of patients who participated to the activity of writing a diary stayed in the centre of care and started a long term pathway of care, reducing the number of “escapes” after the first encounter and contributing to limit the “dr. shopping” phenomenon, which generates a surplus of costs for repetitions of exams and inappropriate visits.
The second important result is the confirmation of the strategic application of Narrative Medicine in building relationships of care in the daily clinical practice. Narrative Medicine can be applied also in contexts of care with lack of time at disposal, like an outpatient of rheumatology. Narrative tools allow to recover the limit of time, creating further spaces for expressions; furthermore, with a regular use of narrative, also the quality of the time during the visits improves, throughout a more flowing and efficient communication.
Tab.1 – The transactions of ego states
This pilot experience can be extended to other contexts of care and Narrative Medicine can represent a bridge not only between patients and doctors, but also between individual and organizational needs.